Professor Brings Insight to Cell Therapy with Nanobots
Research explores how engineered nanoparticles, or nanobots, can serve as watchdogs of cellular health and function

There's an unfortunate irony in cell therapy that holds it back from its full potential: Regenerating tissues often must be damaged to know if the treatment is working, such as surgically removing tissue to see if rejuvenation is occurring beneath.
The alternative isn't much better: Patients can choose to wait and see if their health improves, but after weeks of uncertainty, they might find that no healing has taken place without a clear explanation as to why.
Jinhwan Kim, a new assistant professor of biomedical engineering at the University of California, Davis, who holds a joint appointment with the Department of Surgery at UC Davis Health, wants to change all of that. In his research program, he combines nanotechnology and novel bioimaging techniques to provide non-invasive, real-time monitoring of cellular function and health.
Good Things Come in Small Packages
For his Ph.D. in chemistry from the Pohang University of Science and Technology in South Korea, Kim developed nanobots, or nanoparticles, capable of avoiding the body's natural response to attack foreign invaders.
"In nanoparticle [drug] delivery, the problem is that our body is so smart," Kim said. "I made my nanoparticles smarter so that whenever [they] meet any biological barrier, they change their physical properties to overcome those biological barriers."
This innovative nanotechnology forms the basis of Kim's current research. However, rather than use the nanobots to improve drug delivery like before, he is using them to serve as something like a watchdog for stem cells and immune cells, which are often challenging to track due to their ability to bypass biological barriers in the body.
For example, they can sound the alarm when they detect that a cell is dying — or any other biological event that Kim is interested in. He can build them to be sensitive to specific cellular states or behaviors and to send a signal when it detects signs of them occurring.
To achieve this, he combines one of his engineered nanoparticles with a stem or immune cell. He then injects these engineered cells into a body's circulatory system.
Cellular Communication
Fittingly, to perceive the signals made by his engineered nanoparticles once they are inside someone's body, Kim uses two imaging techniques that rely on sound.
He combines ultrasound, which uses high-frequency sound waves to capture high-resolution images of what's going on inside the body, with photoacoustic imaging — a technique that makes it possible to measure functional aspects like oxygen levels by mixing ultrasonic frequencies with lasers (aka, sound and light).
Together, the imaging techniques give Kim the advantages of traditional optical imaging, which means he can detect light from the entire visible spectrum and penetrate deep into the body without invasive surgery.
They also grant him access to a frequency that nanoparticles use.
"There are many types of nanoparticles that absorb a specific light, and then they create a photoacoustic signal," Kim said. "I basically use those photoacoustically active nanoparticles to engineer [and track] cells."
This new visualization method coupled with his engineered nanorobots may offer the medical insights necessary to advance cell-based cancer immunotherapies and regenerative medicine broadly.
(Jinhwan Kim/UC Davis)

(Matt Marcure/UC Davis)
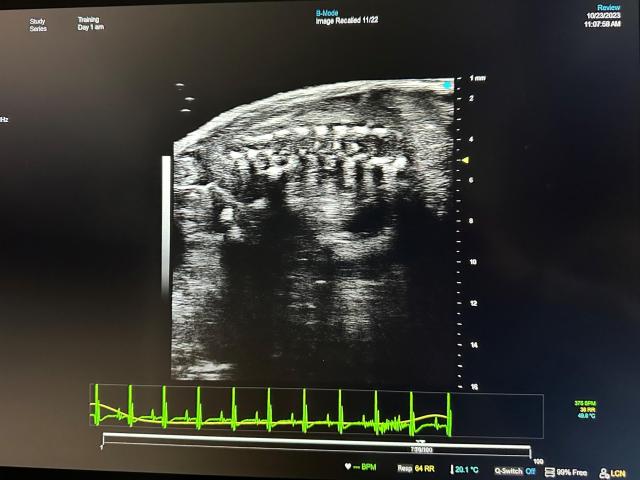
Backbone structure of mouse uterus seen through a high-frequency image, left, created by the transducer on the right. Kim uses this biomedical imaging technique to receive the photoacoustic signals from his nanobots.
The Power of Pictures
The idea to use nanoparticles for non-invasive monitoring of cells came to Kim while he was a postdoctoral research scientist at Georgia Institute of Technology under the supervision of Professor Stanislav Emelianov, a nationally recognized expert in biomedical imaging. Kim was in a discussion about ultrasound and photoacoustic imaging when he suddenly found himself thinking of an illustration he had seen in a magazine years earlier.
"During high school, I really enjoyed reading popular science magazines," he said. "There's a picture that I saw once about really small robot-looking objects [circulating] in our blood. The magazine said, 'This is going to be the future of medicine.'"
That one visual is the genesis of Kim's entire academic career and why he has pursued biomedical engineering, materials science and chemistry — to make what he saw a reality. However, the further he went into his career, the farther he went away from that original inspiration.
Yet, that one discussion and sudden memory synthesized all the research he had done up to that point and brought Kim back to his original goal — and ultimately to his research program looking into stem cell therapy and immunotherapy at UC Davis.
"I'm really happy that my career and my research program came back to what I originally wanted to do," Kim said, "[which is] to create a miniaturized robot that can [help] treat disease, analyze signals and maybe tell us what cells are doing in real-time, non-invasively."
An Exciting Place for Engineers
Kim's lab is based at UC Davis Health in Sacramento, California. The location allows him to be close to his faculty mentor, Professor Aijun Wang, and to teach biomedical engineering courses in the Quarter at Aggie Square program. The courses offer an immersive bench-to-bedside experience for undergraduate students to explore in clinical settings at UC Davis Health.
As an engineer first, Kim says he was anxious about being stationed on a medical campus but now finds it to be one of the most exciting parts of his joint appointment between the Department of Surgery and the Department of Biomedical Engineering.
"It's only been three months, but I already feel a big discrepancy between what engineers know versus what the medical field is doing. I think this is a really great opportunity for me to find out the medical problems and solve or provide an engineering solution to them — to make human health care better."
